Part A — Maternal-Infant Data Standards Framework
The Problem
- Separate maternal and infant EHR systems prevent clinicians from seeing the full dyad picture when treating substance-exposed families.
- Critical dyad-specific details—maternal treatment plans, infant NAS scores, social services involvement—lack consistent standardized fields.
- Privacy regulations and lagging claims data slow information exchange, leaving care teams without timely, shareable context.
The Solution
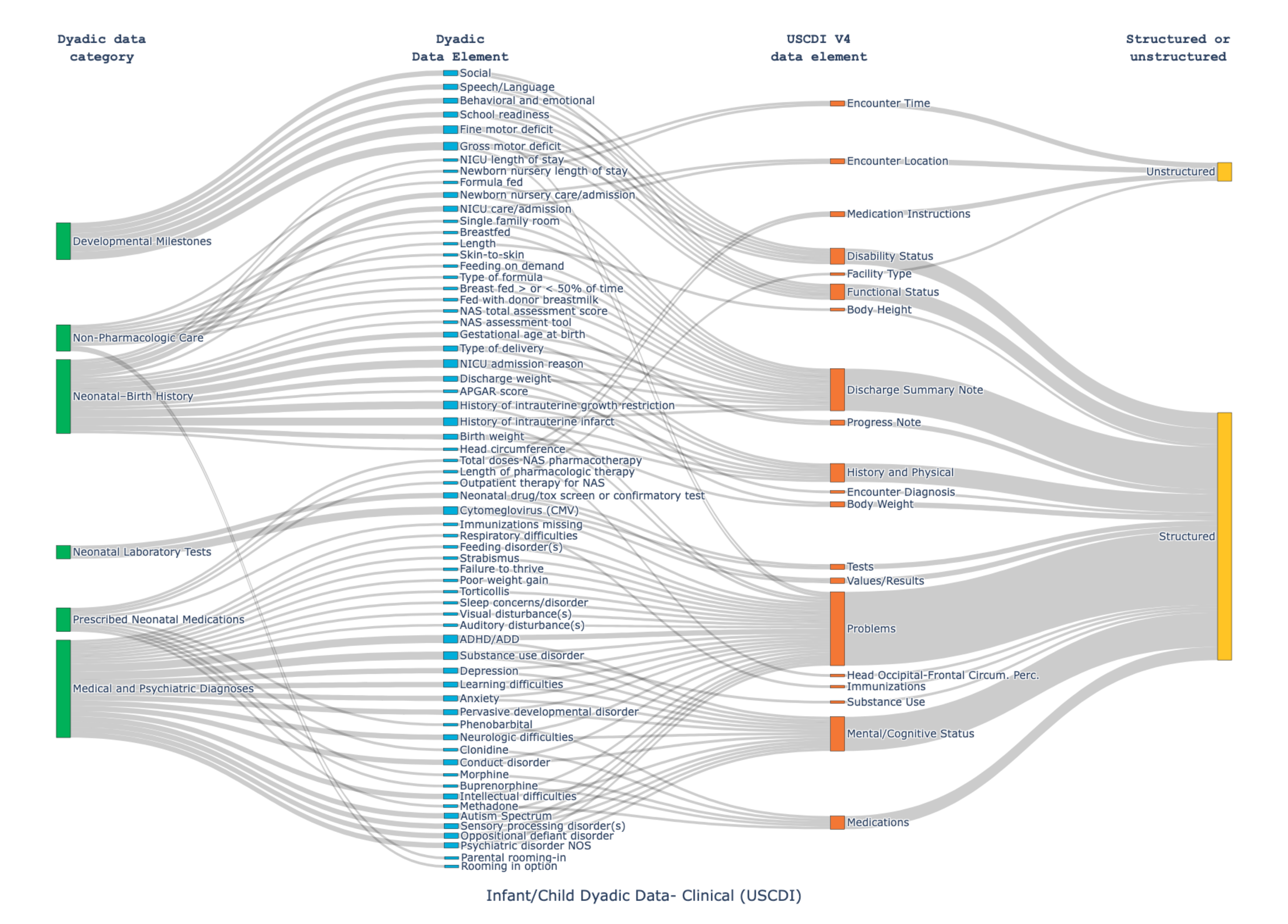
- Catalogued 180 clinical and social data elements essential to dyad care and mapped each to USCDI and FHIR definitions to quantify coverage.
- Surveyed HIEs and hospitals to understand current mother–infant linkage practices and adoption of national interoperability standards.
- Authored recommendations to close standard gaps and accelerate adoption, guiding agencies on data elements to prioritize for dyad coordination.
Architecture Overview
- Combined manual expert review with Python-assisted lookups to align each dyad element to standard vocabularies without missing edge cases.
- Designed and analyzed a structured HIE survey, blending quantitative aggregations with qualitative insights on linkage maturity.
- Visualized coverage and gaps through Sankey charts and coverage dashboards to clearly communicate where standards succeed.
- Validated mappings with neonatologists, addiction specialists, and informaticians to ensure semantic accuracy before publication.
- Documented integration pathways so future tools can rely on the mapped standards, laying the groundwork for operational dashboards.
Results and Impacts
- Proved that a majority of dyad data needs are already covered by national standards, reducing perceived technical barriers for health systems.
- Published findings in JAMIA, giving implementers a vetted reference for configuring systems that track maternal-infant outcomes.
- Informed ONC equity guidance and an HHS “Dyad Data Tracker” initiative that uses the mapped elements to monitor outcomes.
Skills and Tools Used
| Technique/Skill | Tools/Implementation |
|---|---|
| Healthcare Data Standards | Deep expertise in USCDI v4 and FHIR R4; mapped custom dyad requirements to standard fields to ensure semantic alignment. |
| Data Mapping & Scripting | Combined spreadsheets with Python automation to catalog 180 elements and track coverage versus gaps. |
| Survey Design & Analysis | Crafted targeted HIE surveys and analyzed responses to understand real-world linkage capabilities. |
| Stakeholder Collaboration | Coordinated with ONC, HHS, and clinical partners, translating technical findings into actionable policy guidance. |
| Data Visualization | Built Sankey diagrams and coverage dashboards to communicate mapping outcomes to decision-makers. |
| Domain & Regulatory Knowledge | Navigated NAS scoring, maternal OUD care, HIPAA, and 42 CFR Part 2 to ensure recommendations fit real-world constraints. |
Cross-Project Capabilities
- Demonstrated standards-first solution design, a practice applied across subsequent interoperability and surveillance projects.
- Bridged policy and engineering, ensuring technical solutions align with national health IT initiatives.
- Modeled a rigorous discovery approach that informs later ML deployments, from ICU analytics to equity dashboards.
Published Papers/Tools
- Journal of the American Medical Informatics Association (2025): detailed mapping of dyad data elements to USCDI/FHIR.Paper
- Public supplementary spreadsheet cataloging all 180 elements and their standard codes for implementers.
Part B — Maternal-Infant Dyad Care Dashboard Prototype
The Problem
- Mother and infant records live in different systems, forcing clinicians to toggle across interfaces and risking missed context during fast-moving care decisions.
- Key maternal information is often buried in long notes, making it difficult to correlate with infant withdrawal trends.
- Cross-disciplinary teams rely on manual updates, so actionable dyad intelligence rarely reaches the bedside in time.
The Solution
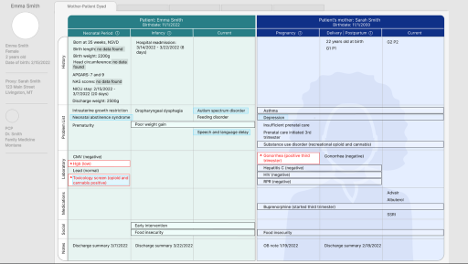
- Designed a SMART-on-FHIR application that pulls authenticated data for linked mother–infant pairs into a unified, parallel layout.
- Collaborated with OB, NICU, and social work stakeholders to prioritize content and interaction patterns that match dyad workflows.
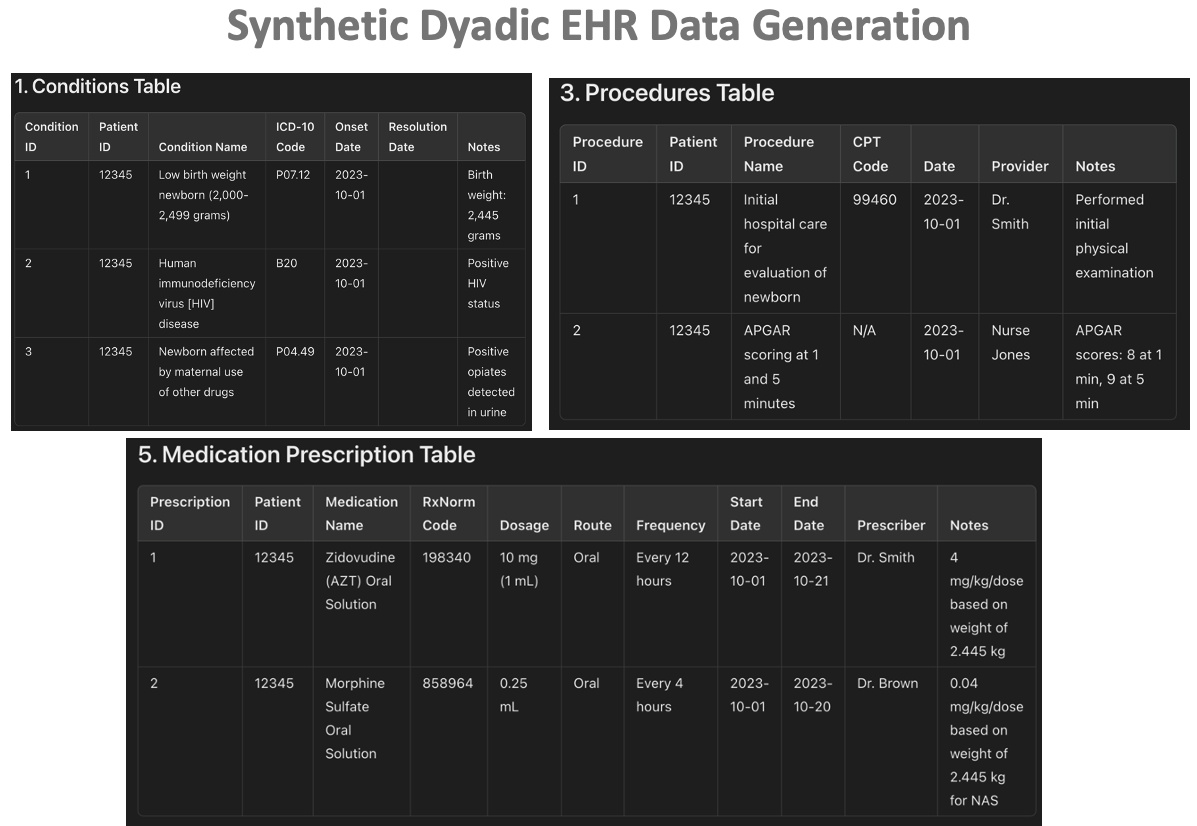
- Populated the prototype with realistic synthetic data to demonstrate core use cases—e.g., comparing maternal toxicology results with infant NAS trajectories.
Architecture Overview
- Iterated low- to high-fidelity designs in Balsamiq and Figma, grounding interface choices in clinician journey mapping.
- Implemented the front end with HTML, CSS, and JavaScript.
- Queried FHIR resources—medications, labs, vitals—for both mother and infant, using shared identifiers to pair records in real time.
- Generated synthetic dyad datasets with GPT-4 and custom scripts to test the interface under realistic clinical scenarios.
- Ran usability walkthroughs with clinicians, adjusting layout and highlighting logic based on observation and feedback.
Results and Impacts
- Clinicians immediately saw the benefit of seeing maternal context alongside infant NAS scores, validating the design direction.
- Stakeholders across HHS and hospital leadership endorsed advancing to a pilot, citing the prototype as proof of feasibility.
Skills and Tools Used
| Technique/Skill | Tools/Implementation |
|---|---|
| UI/UX Design | Led user-centered design with wireframes and high-fidelity prototypes tailored to dual-patient views. |
| Web Development | Built the SMART-on-FHIR front end with HTML, CSS, and JavaScript for secure deployment inside the EHR. |
| FHIR API Integration | Queried medications, labs, vitals, and notes for linked patients using OAuth2-authenticated FHIR calls. |
| Synthetic Data Generation | Created realistic dyad datasets with GPT-4 and custom scripts to test workflows without exposing PHI. |
| Usability Testing | Conducted iterative clinician walkthroughs, capturing insights that shaped layout and alert logic. |
| Product & Project Leadership | Orchestrated multi-phase development, aligning designers, engineers, and clinical advisors under agile cadences. |
Cross-Project Capabilities
- Reinforced ability to synthesize disparate data streams into unified experiences, echoed in biosurveillance and ICU projects.
- Showcased the fusion of AI outputs with clinician-friendly UX, a throughline for bedside decision-support work.
- Highlighted cross-disciplinary leadership, guiding teams from concept through demonstrable prototypes.
Published Papers/Tools
- Internal report and demo video distributed to HHS opioid policy leaders outlining architecture and usability findings.
- Planned AMIA/HIMSS submissions describing the standards-driven design approach and early clinician feedback.
- Open-source prototype code (with synthetic FHIR data) released to encourage adoption and iteration by other health systems.
- Featured in national health IT briefings and newsletters as a forward-looking example of dyad-centered care.